Percutaneous Antibiotic Delivery Technique (PAD-T)
The PAD-T was developed in 2009 by Dr. Karr and used extensively as a safe, extremely effective means utilizing a bone void filler consisting of calcium sulfate and phosphate with antibiotic into an area of bone infection. The PAD-T involves a small percutaneous skin incision followed by a small bone cortex incision into the infected bone. Irrigation and spongiosum bone cultures can be done through the bone cortex incision. The procedure is done in the operating room and the patient can generally weight bear afterwards. This technique avoids a more invasive bone surgery, thus this minimizes time away from work, and generally requires no change in weight bearing status.
A closed bone infection has the cortical bone intact without bone collapse without septic arthritis. A simple percutaneous skin incision is completed near to the area of osteomyelitis. The bone cortex incision is made with either a steinmann pin as close in diameter to the kyphon delivery device as possible to allow a snug purchase of the kyphon needle to the bone cortex or a Jamshedi needle to minimize BVF leakage. This tight purchase between the bone and the delivery device cannot be over emphasized. If a bone cortex incision is made that the delivery device is loose at the bone conical surface, the bone void filler with antibiotic (BVFA) will leak out at the bone cortex incision and not travel completely into the bone. The delivery device is then advanced to the far bone cortex without far bone cortex violation. Usually a single plane pass of the delivery device is sufficient. Multiple passes can unnecessary increase the risk of stress risers with fracture and should be avoided. After the bone cortex incision is completed, bone irrigation and biopsies for culture can be completed with a curved curette. For all lower leg, tarsal, and lesser tarsal bones use a number three kyphon needle. For the smaller bones, i.e. phalanxes and metatarsals, a number two kyphon needle is used. A Jamshedi needle can be used when the bone surface is deep to the skin of the bone is small. However, when using a Jamshedi needle, you will not be able to take a bone culture.
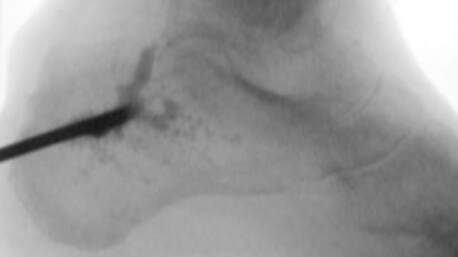
Under intra-operative fluoroscopy the delivery device is then advanced through the bone cortex incision into the spongiosa bone. The kyphon needle is then slowly withdrawn under intra-operative fluoroscopy while delivering the BVFA. Under intra-operative fluoroscopy there should be a nice filling effect seen as the BVFA fill the infected bone. Stop injecting when the bone defect when you meet resistance in placing the BVFA into the bone, i.e. there is product ooze through the bone cortex incision, small cortical defects, or some product is seen in the soft tissue or vasculature on intra-operative fluoroscopy. Stop when you visualize any product in the vasculature. You do not need to place a lot of BVFA to be successful, especially in small bones. In a smaller void or small bone, only 1-2 cc's of product is needed. In the situation where a two-plane delivery is planned, after the first pass of the BVFA, the percutaneous soft tissue incision should be closed before the second pass is initiated. This is done so there is no leakage out of the first cortex bone incision from the second pass. Even though the delivery BVFA is not cytotoxic in vitro to fibroblast, a large amount of BVFA into soft tissues may cause an immune reaction, compartment syndrome, or excessive leakage through the incision or ulcer.
A closed bone infection has the cortical bone intact without bone collapse without septic arthritis. A simple percutaneous skin incision is completed near to the area of osteomyelitis. The bone cortex incision is made with either a steinmann pin as close in diameter to the kyphon delivery device as possible to allow a snug purchase of the kyphon needle to the bone cortex or a Jamshedi needle to minimize BVF leakage. This tight purchase between the bone and the delivery device cannot be over emphasized. If a bone cortex incision is made that the delivery device is loose at the bone conical surface, the bone void filler with antibiotic (BVFA) will leak out at the bone cortex incision and not travel completely into the bone. The delivery device is then advanced to the far bone cortex without far bone cortex violation. Usually a single plane pass of the delivery device is sufficient. Multiple passes can unnecessary increase the risk of stress risers with fracture and should be avoided. After the bone cortex incision is completed, bone irrigation and biopsies for culture can be completed with a curved curette. For all lower leg, tarsal, and lesser tarsal bones use a number three kyphon needle. For the smaller bones, i.e. phalanxes and metatarsals, a number two kyphon needle is used. A Jamshedi needle can be used when the bone surface is deep to the skin of the bone is small. However, when using a Jamshedi needle, you will not be able to take a bone culture.
Under intra-operative fluoroscopy the delivery device is then advanced through the bone cortex incision into the spongiosa bone. The kyphon needle is then slowly withdrawn under intra-operative fluoroscopy while delivering the BVFA. Under intra-operative fluoroscopy there should be a nice filling effect seen as the BVFA fill the infected bone. Stop injecting when the bone defect when you meet resistance in placing the BVFA into the bone, i.e. there is product ooze through the bone cortex incision, small cortical defects, or some product is seen in the soft tissue or vasculature on intra-operative fluoroscopy. Stop when you visualize any product in the vasculature. You do not need to place a lot of BVFA to be successful, especially in small bones. In a smaller void or small bone, only 1-2 cc's of product is needed. In the situation where a two-plane delivery is planned, after the first pass of the BVFA, the percutaneous soft tissue incision should be closed before the second pass is initiated. This is done so there is no leakage out of the first cortex bone incision from the second pass. Even though the delivery BVFA is not cytotoxic in vitro to fibroblast, a large amount of BVFA into soft tissues may cause an immune reaction, compartment syndrome, or excessive leakage through the incision or ulcer.